Circulating plasma proteomics analysis of CMV infection in kidney transplantation
Tara Sigdel1, Patrick Boada1, David Gjertson3, Elaine F Reed3, Maura Rossetti3, Joanna Schaenman3, Hanno Steen2, Benoit Fatou2, Suphamai Bunnapradist3, Minnie Sarwal1.
1UCSF, San Francisco, CA, United States; 2Harvard Medical School, Boston, CA, United States; 3UCLA, Los Angeles, CA, United States
Purpose: Cytomegalovirus (CMV) infection is a threat to kidney transplantation. We studied circulating host proteome perturbations due to CMV infection in kidney transplantation as it could provide further insight on CMV infection and pathogenesis.
Methods: We performed LC-MS-based proteomics using 168 plasma samples collected pre- and longitudinally post-CMV viremia from 62 propensity score-matched UCLA kidney transplant patients of which 31 were CMV positive and 31 were CMV -ve. Recipients were sampled 3 and 12 months after transplant, with additional samples 1 week and 1 month after viremia. All data were log2 transformed for the analysis. Differential expression analysis was conducted by using R and Limma. T-tests were conducted by using the built-in statistics functionality in the R environment.
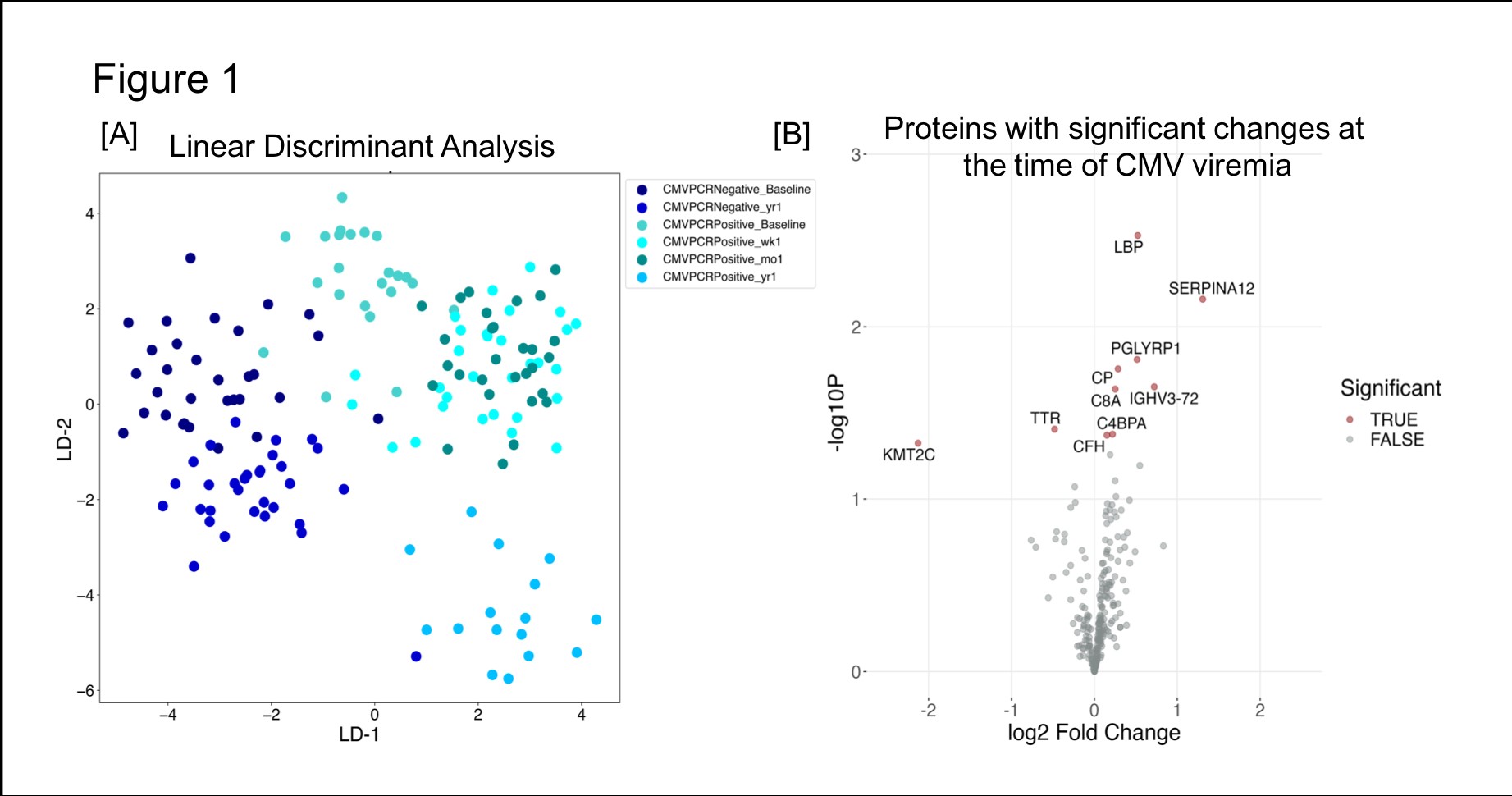
Results: Using Linear Discriminant Analysis, protein profiles with 241 plasma proteins were able to separate samples based on CMV viremia status and based on post-viremia time (Fig1A). Analysis of plasma proteins at the baseline pre-infection resulted in a set of 17 proteins whose levels were either increased (n=6) or decreased (n=11). The most significantly increased protein was Lysine Methyltransferase 2C (KMT2C) with 3.38 fold increase (p=0.05) in CMV+ve samples and most significantly decreased protein was Immunoglobulin Lambda Variable 7-43 (IGLV7-43) with 2.17 fold decrease (p=0.01). The significant proteins were enriched in plasminogen activation and blood coagulation pathways as the top two biological pathways. The protein profile of baseline samples of CMV +ve patients was compared with protein profiles of 1-week post-viremia samples which resulted in ten significantly changed proteins (p<0.05). The significant proteins' expression direction and significance are presented as a volcano plot (Fig1B). Increased proteins at the time of CMV+ve viremia (1-week post-viremia) included Serpin Family A Member 12 (SERPINA12) with p-value 0.01 and 2.47 fold increase and Immunoglobulin Heavy Variable 3-72 (IGHV3-72) with p-value 0.02 and 1.65 fold increase. Transthyretin (TTR ) and Lysine Methyltransferase 2C (KMT2C). CMV-specific proteins were enriched with functions such as protein activation cascade (p=1.42E-06) and regulation of acute inflammatory response (p=0.0001).
Conclusions: We have identified plasma proteins that strongly correlate with CMV viremia in kidney transplantation and provide an insight about biological changes due to CMV viremia.

right-click to download
