Dapsone induced hemolytic anemia in solid organ transplant recipients with normal G6PD activity
Walaa Dabbas1, Ruchi Naik1, Ignatius Tang1.
1Nephrology, University of Illinois at Chicago, Chicago, IL, United States
Purpose: Pneumocystis jirovecii Pneumonia (PJP) is a life-threatening infection in solid organ transplant recipients. Trimethoprim-sulfamethoxazole (TMP-SMX) is the first line regimen. For people who are intolerant to TMP-SMX, Dapsone is a commonly used alternative. G6PD deficiency should be ruled out before initiation of Dapsone to avoid hemolytic anemia. However, Dapsone associated hemolytic anemia with normal G6PD activity has been reported in HIV patients as well as solid organ transplant recipients. We present a case series of 6 transplant recipients who developed hemolytic anemia after initiation of Dapsone despite normal G6PD activity.
Methods: We identified 6 organ transplant recipients with normal G6PD activity who developed anemia after initiation of Dapsone for PJP prophylaxis. Anemia workup include iron studies, vitamin B12, folate, reticulocyte count, haptoglobin, LDH, gastrointestinal, and other anatomic blood loss.
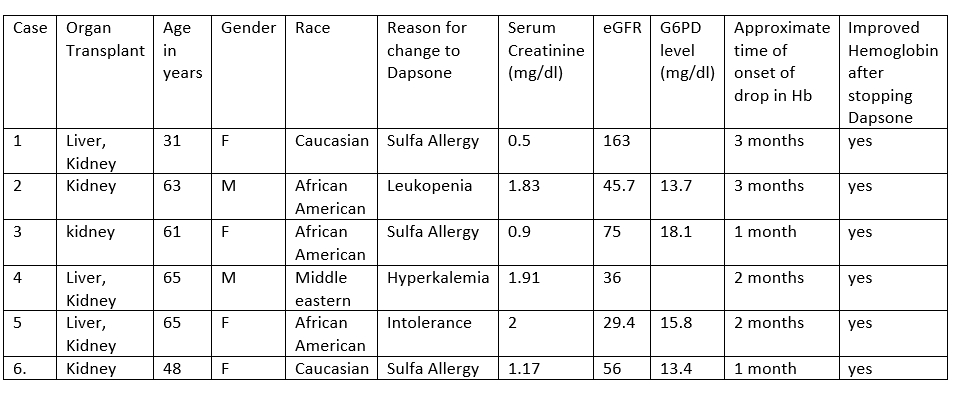
Results: All 6 patients had elevated reticulocyte count consistent with hemolytic anemia. Two patients had persistently low haptoglobin but no other signs of microangiopathic hemolytic anemia. There was no substrate deficiency or blood loss. After discontinuation of Dapsone, hemoglobin improved back to baseline without blood transfusion. For summary of cases, see Table.
Conclusions: Dapsone associated hemolytic anemia can occur in solid organ transplant recipient with normal G6PD activity. It is important to monitor hemoglobin within the first 3 months of Dapsone initiation. Blood transfusion is usually not required. The pathophysiology of Dapsone associated hemolytic anemia requires further studies.

right-click to download
