Extended criteria donor, cold ischemia time and delayed graft functions; common ingredients for an expensive recipe
Mohamed zahran1,2, Francesca Leonardis 3, Ismail Mohamed4, Evaldo Favi5, Roberta Angelico 3, Tommaso Manzia3, Giuseppe Tisone3, Roberto Cacciola2,3.
1Urology department, Urology and Nephrology Center, Mansoura University, Egypt, Mansoura, Egypt; 2Surgery department, King Salman Armed force hospital, Tabuk, Saudi Arabia; 3Department of Surgical sciences, Tor Vergata University, Rome, Italy; 4Renal Transplant Unit, Royal London Hospital, London, United Kingdom; 5Department of General Surgery and Renal Transplantation, Fondazione Ca’ Granda Ospedale Maggiore Policlinico, Milano, Italy
Introduction and objectives: Delayed Graft Functions (DGF) has a relevant impact in Kidney Transplantation (KTx) being associated with suboptimal outcomes and increased healthcare costs. The necessary and increased use of Extended Criteria Donors (ECD) is inevitably linked with more DGF. Cold Ischemia Time (CIT) remains a crucial determinant of DGF. In the UK specific standards of CIT have been established for KTx from Donors after Brain Death (DBD), <18 hours and Donors after Circulatory Death (DCD) <12 hours. In this study we evaluate the incidence and impact of Beyond Standard (BS) CIT in ECD and estimate the cost of DGF in this group of recipients of KTx.
Material and methods: We retrospectively reviewed our database with 218 consecutive KTx and analyzed type of donors, donor characteristics, incidence of DGF and Primary Non Functions (PNF). We also analyzed the CIT and its component defined as Extraction Time (ET) Transport Time (TT) and time from Delivery of the Kidney to Perfusion with Blood called Unit Time (UT). The cost estimate of the impact of DGF was based on the tariff for KTx currently paid by Healthcare Commissioners (HC) in the UK equivalent to £17,000. The cost estimate of DGF was based on available published evidence identifying an increased 10% for hospitalization and further 10% for dialysis sessions >1.
Results: There were 103 (47.2%) KTx from ECD, of whom with a BS CIT were 37/103 (35.9%). Overall, in the ECD group DGF/PNF was observed in 47/103 (45.6%) patients. The incidence of DGF/PNF in ECD KTx with a BS CIT was 22/37 (59.5%) compared with 25/66 (37.9%) in those ECD transplanted Within Standard (WS); CIT (P=0.03). The major component of CIT was UT, representing 70%±15% of the CIT.
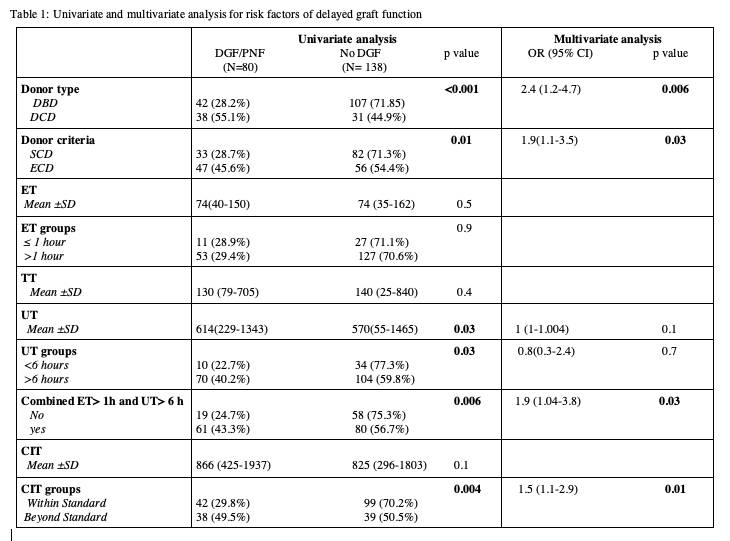
There were 115 (52.8%) KTx from SCD, of whom with a BS CIT were 40/115 (34.8%). Overall in the SCD group DGF/PNF was observed in 33/115 (28.7%) patients. The incidence of DGF/PNF is SCD KTx with a BS CIT was 16/40 (40%) compared with 17/75 (22.7%) in those SCD transplanted Within Standard (WS) CIT (P=0.04). The major component of CIT was UT representing 65%±18% of the CIT. Univariate and multivariate analysis of risk factors of DGF is illustrated in table 1.
Cost estimate: In the ECD group, we calculated £151.300 increase of the total cost. The Individual KTx had a mean ±SD cost in BS CIT and WS CIT of £19543.2 ±2173.9 and £18503± 2034 (p=0.01). Similarly, in the SCD group, we calculated £110.500 increase of the total cost. The Individual KTx had a mean ±SD cost in BS CIT and WS CIT of £18692.5 ±2140.6 and £17997.3± 1854.4 (p=0.07). Overall, the total increase of the cost was £261800 and the mean ±SD cost in BS CIT and WS CIT was £19543.2± 2173.9 and £18503 ±2034 (p=0.01).
Conclusion: Our series shows that a substantial proportion of KTx have been performed with a BS CIT which certainly influences the incidence of DGF and PNF in KTx especially from ECD and consequently increases the estimate cost. Adequate infrastructure and readiness of all transplant facilities in order to reduce CIT are mandatory for accepting ECD.

right-click to download
