Incidence and associated factors with uncontrolled hypertension at 12- months post-renal transplantation
Ziad Arabi1,2,3, Mubarak Abdalla1,2,3, Elwaleed Elhassan1,2,3.
1Division of Nephrology, Department of Medicine, King Abdulaziz Medical City, Riyadh, Saudi Arabia; 2King Abdullah International Medical Research Center, Riyadh, Saudi Arabia; 3College of Medicine, King Saud Bin Abdulaziz University for Health Sciences, Riyadh, Saudi Arabia
Background: Uncontrolled hypertension (HTN) after renal transplantation is not uncommon. However, our center has not studied its incidence and risk factors post kidney transplantation before.
Method: A single-center retrospective study of the renal transplant recipients who underwent kidney transplantation between January 2017 to May 2020 with12 months of follow-up. The goal target of hypertension treatment during this retrospective study was <140/90 mmHg as per the published guidelines at that time. We divided patients according to their blood pressure (BP) control at 12 months post kidney transplantation into two groups: controlled BP ( ≤140/90) and uncontrolled BP( > 140/90). We studied the association between the patients’ demographics and baseline cardiovascular risk factors and uncontrolled HTN 12 months post kidney transplantation. We also studied the association between pretransplant (baseline) cardiovascular imagings and uncontrolled HTN at 12 months. These tests included:(ejection fraction, wall motion abnormalities on echo, calcium scoring, perfusion stress test, cardiac angiogram, and the degree of calcifications on CT of pelvic arteries). Additionally, we studied the changes seen during the first 12 months post kidney transplantation. These included: creatinine change, rejection, weight change, A1C change, post-transplant diabetes, LDL change, PTH change from baseline, and persistent hyperthyroidism.
Results: A total of 254 renal transplant recipients were included. 74% were ≥ 30 years, 58% were men, and 80% were living-donor kidney recipients. Preemptive transplantation was 10.1%, PD: 11.5% and HD: 78.4%.
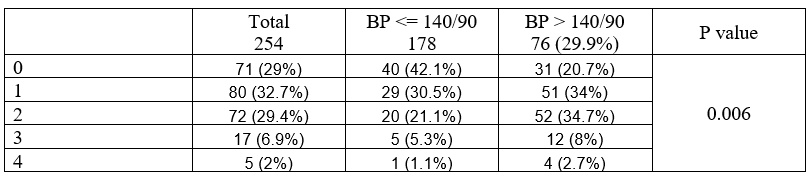
At one year, 76 (29.9%) of the patients did not attain the BP goal of 140/90. SBP decreased from baseline to 12 months by -7.2±18.6 mmHg in the group with controlled BP and whereas it increased by 3.5±16.9 mmHg in the group with uncontrolled BP. (P:<0.001). DBP decreased from baseline to 12 months by -4.1±12 mmHg in the group with controlled BP, whereas it increased by 2±13.7 mmHg in the group with uncontrolled BP (P<0.001). Among characteristics and baseline cardiovascular risk factors, factors associated with uncontrolled HTN included age (47 VS 41 years, P:0.008) and DM (P:0.012). Whereas gender, dialysis vintage, preemptive transplantation, type of dialysis (hemodialysis VS peritoneal dialysis), type of transplant (living donor kidney transplant VS deceased donor kidney transplant), and smoking were not different among the two groups. None of the pre-transplant (baseline) cardiovascular imaging findings were associated with having uncontrolled BP >140/90 at 12 months. Similarly, there was no association between uncontrolled HTN and creatinine change from baseline, rejection, weight change, A1C change, post-transplant diabetes, LDL change, PTH change from baseline, and persistent hyperthyroidism. However, higher BMI at 12 months was associated with a higher incidence of uncontrolled HTN (BMI 27.2±5.9 vs. 29.2±5.4, P: 0.013). Multivariate analysis showed that the predictors of uncontrolled blood pressure (>149/90 mmHg) included a higher creatinine (OR=1.016, CI=1.004-1.028. p=0.01) and smoking (OR=3.58, CI=1.001-12.8. p=0.05).
Conclusion: At one-year post renal transplantation, about one-third (29.9%) of the renal transplant recipients had uncontrolled hypertension despite multiple BP medications. SBP and DBP significantly trended up from baseline after transplantation in those with uncontrolled hypertension. In contrast, SBP and DBP significantly decreased from baseline after transplantation in those with controlled hypertension. This interesting finding requires further confirmation by a controlled prospective study.

right-click to download
