Performance of the hypotension prediction index in living donor liver transplant recipients: a prospective observational study
Seong Mi Yang1, Hye-Yeon Cho1, Hyung Chul Lee1, Hee-Soo Kim1.
1Department of Anesthesiology and Pain Medicine, Seoul National University Hospital, Seoul, Korea
Background: The hypotension prediction index (HPI), derived from various features of the arterial waveform, was recently introduced and clinically validated in various surgical conditions.
Objective: To evaluate the performance of HPI in living donor liver transplantation recipients.
Design: Prospective observational study.
Setting: Tertiary hospital, Republic of Korea, from August 2021 to January 2022.
Patients: Twenty adult patients undergoing living donor liver transplantation were enrolled.
Intervention: HPI was monitored via a radial artery catheter during liver transplantation.
Main outcome measures: The mean arterial pressure and HPI were recorded from the end of anaesthetic induction until the end of surgery at 1-minute intervals. The area under the curve (AUC) of the receiver operating characteristic curve was calculated to show the performance of HPI at 5, 10, and 15 min for the whole dataset and in each phase of liver transplantation.
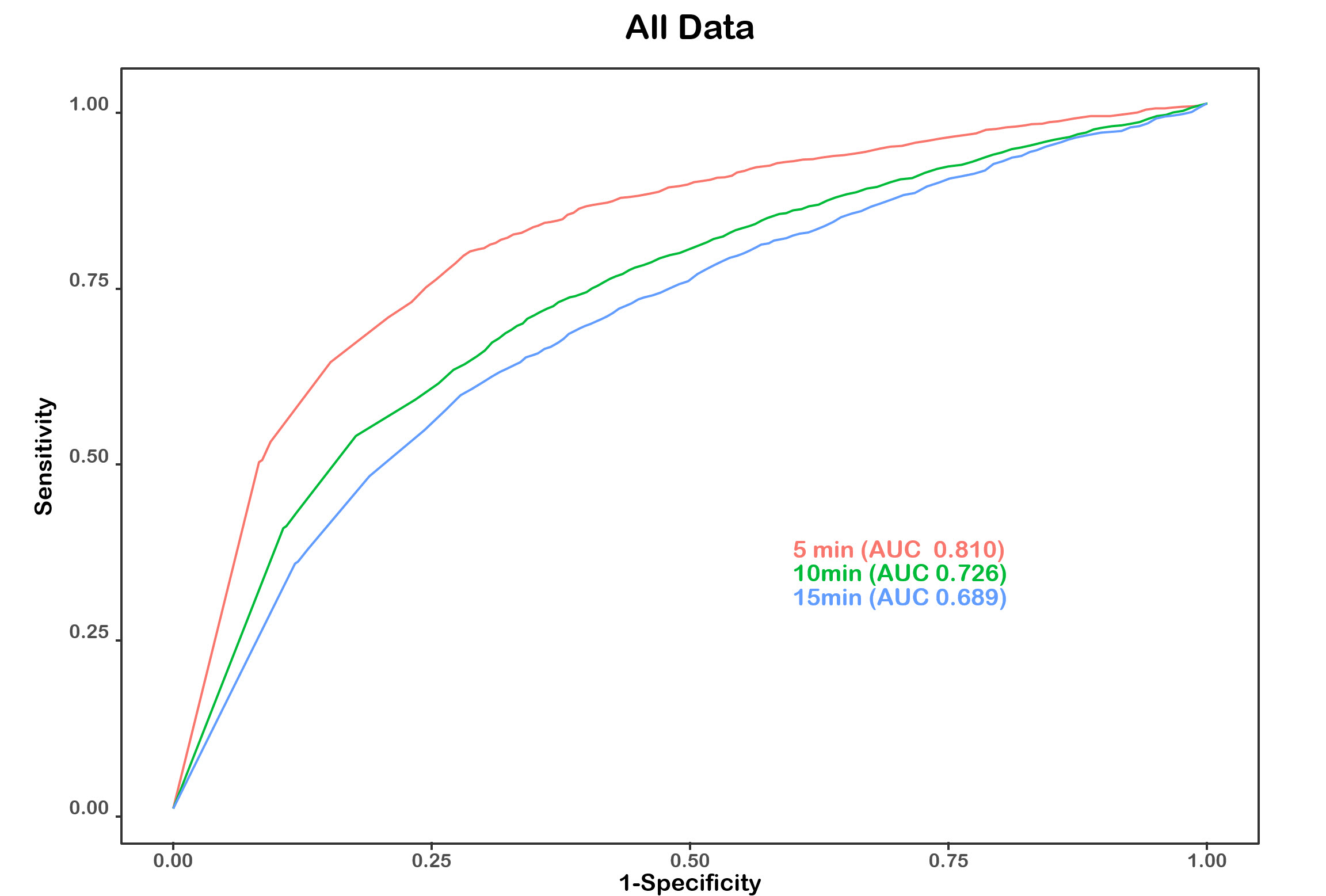
Results: The AUCs for predicting hypotension in the consecutive 5, 10, and 15 min were 0.810 (95% confidence interval [CI]: 0.802–0.818), 0.726 (95% CI: 0.716–0.735) and 0.689 (95% CI: 0.679–0.699), respectively.
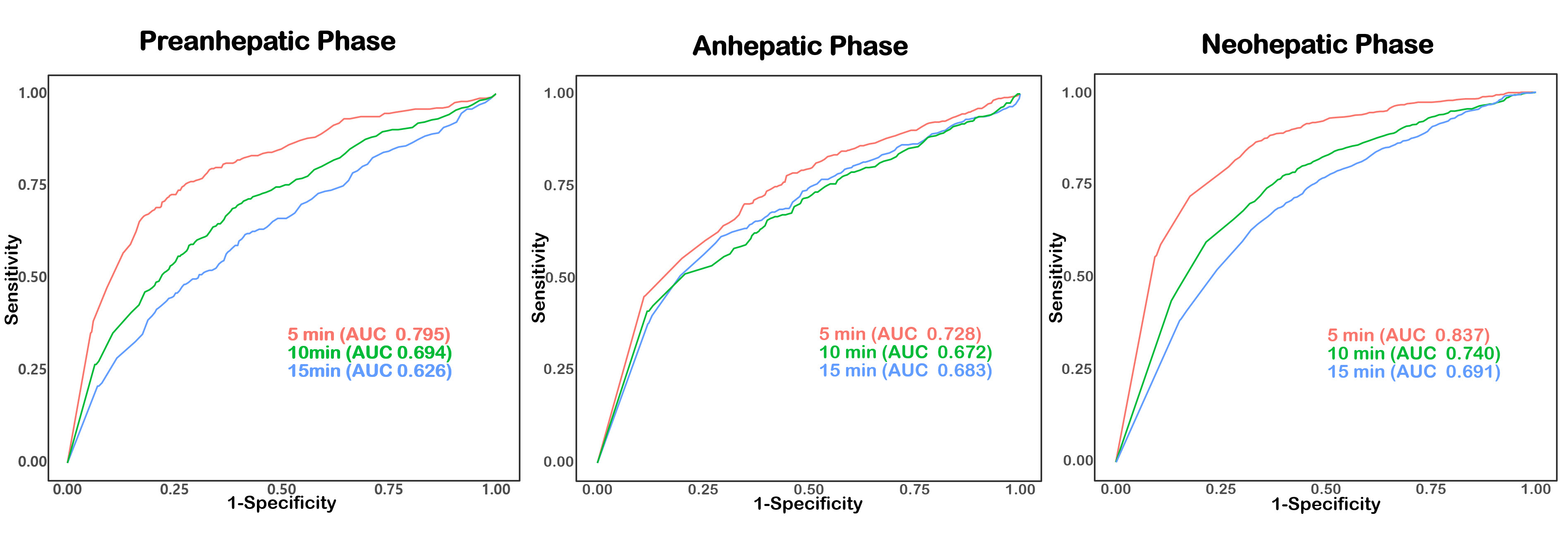
In the preanhepatic phase, the AUCs in the 5-, 10-, 15-min windows were 0.795 (95% CI: 0.780–0.810), 0.694 (95% CI: 0.677–0.711), and 0.626 (95% CI: 0.608–0.645), respectively. In the anhepatic phase, the AUCs in the 5-, 10-, 15-min windows were 0.728 (95% CI: 0.706–0.749), 0.672 (95% CI: 0.649–0.694), and 0.683 (95% CI: 0.660–0.705), respectively. In the neohepatic phase, the AUCs in the 5-, 10-, 15-min windows were 0.837 (95% CI: 0.826–0.848), 0.740 (95% CI: 0.727–0.753), and 0.691 (95% CI: 0.677–0.704), respectively.
Conclusions: HPI can be used as an aid in the hemodynamic management of patients undergoing liver transplantation. Predictability was the highest in the neohepatic phase and the lowest in the anhepatic phase.
This study was supported by the Korea Medical Device Development Fund grant, funded by the Korean Government (Ministry of Science and ICT, Ministry of Trade Industry and Energy, Ministry of Health & Welfare, and Ministry of Food and Drug Safety) (project number: 202011B23).

right-click to download
